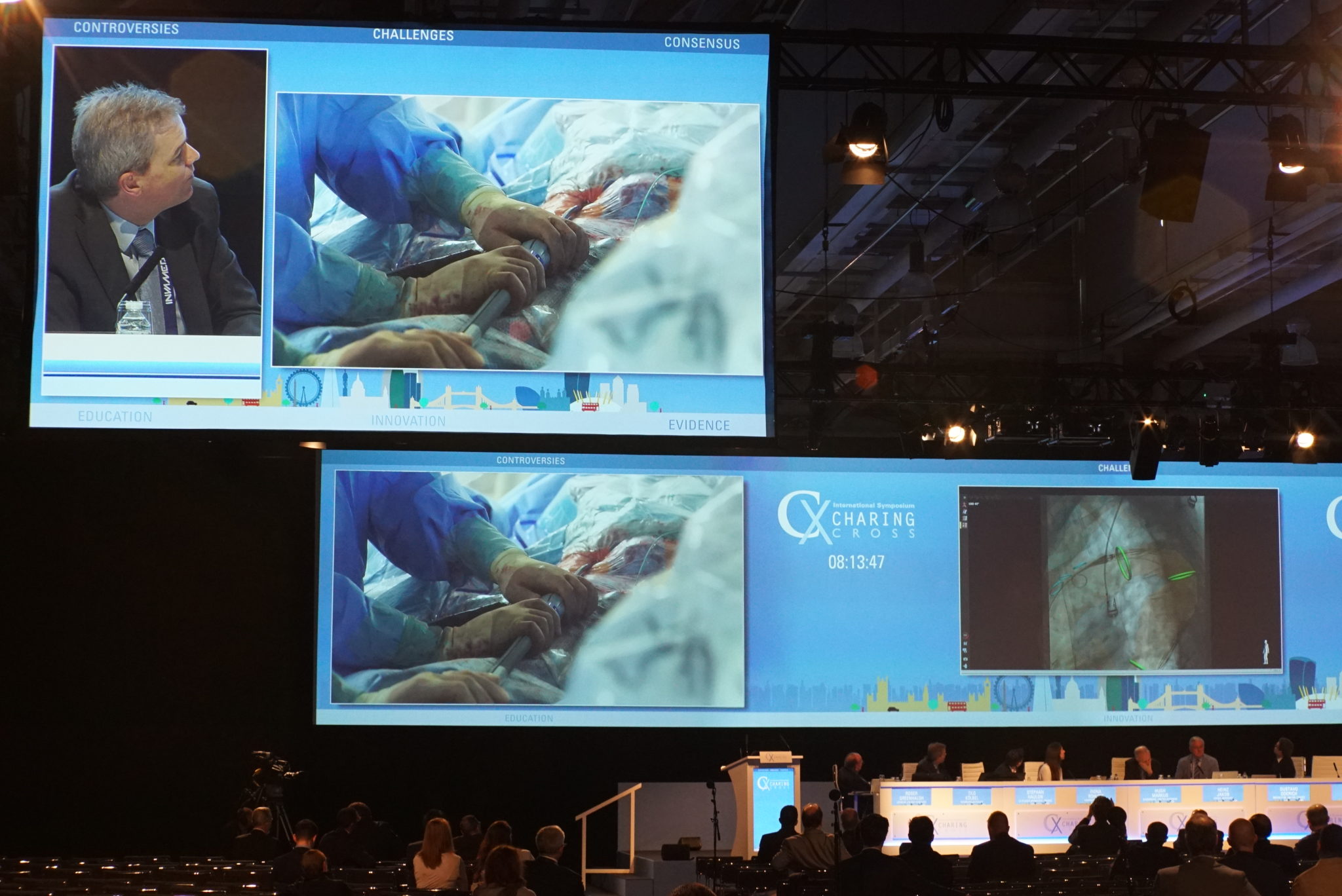
Tilo Kölbel’s team, led on site in Hamburg, Germany, by Giuseppe Panuccio, successfully performed a thoracic endovascular aortic repair (TEVAR) on a 77-year old female patient with American Stroke Association (ASA) class III, and multiple aortic aneurysm disease with multiple aneurysms. The live case was viewed by delegates at Charing Cross (CX) with virtual reality 360° video. The introduction of this visual presentation allowed Kölbel to control the angle and direction of the camera from his seat on the moderating panel at CX, with the ability to show the audience each corner of the operating room in real time. Through discussion of the planning and technique of the repair, the procedure demonstrated best practice for minimising stroke from TEVAR and illustrated an important topic of the main Thoracic Aortic Challenges programme.
“In the aortic arch”, the operators noted, “the thoracic aortic aneurysm is approximately 5cm, and the additional abdominal aortic aneurysm is approximately 4cm.” The team planned the technical procedure to use a two-component Valiant Navion (Medtronic) endograft for the thoracic aneurysm, covering 286mm of aortic arch. “We have a difficult access, because the access vessels are compressed on both sides, so we decided to get our main access on the right side due to the patient’s urostomy and femoral distal bypass on the left side”, they explained, adding that the patient had high-grade stenosis of the right internal iliac artery. As operators had determined the patient was at high risk for spinal cord ischaemia, she received cerebrospinal fluid drainage pre-procedurally, “and we are planning on treating her internal iliac stenosis on the right side.”
The flexibility allowed by the mounted 360° camera allowed for a degree of virtual reality, as viewers were immersed into the Hamburg operating room. Kölbel turned the camera to show the preparative work, as operators and assistants showed the assembling of their tools.
Importantly, as pointed out by Kölbel, flushing of the device with CO2 was performed for two minutes, followed by standard saline flushing. This technique has been highlighted by the Stroke from Thoracic Endovascular Procedures (STEP) study collaborators as a preventative measure to reduce risk of stroke from air embolisation. Chairing the session, Roger Greenhalgh similarly commented “it is important to note that every effort is now being made to exclude air from the system before devices are put into the patient—as that itself can be the cause of stroke by air blockage.” This is a finding presented by Kölbel and Fiona Rohlffs (Hamburg, Germany) at last year’s CX Symposium.
Panucci and the rest of Kölbel’s team swiftly and successfully completed the aortic arch repair, deploying both devices in their planned landing zones. Stéphan Haulon (Le Plessis Robinson, France), co-moderating from the panel, pointed to the importance of large overlaps between multiple devices in this type of procedure. “This is routine now, but a bit different to what we were doing ten or fifteen years ago”, Haulon said. In aneurysmal disease, it has been learned that the diseased aorta will grow not only in diameter, but will continue to grow over time in length as well, as Kölbel commented: “So you need some additional length in order to avoid device separation: when we can, we plan at least three stents’ overlap.” Haulon agreed that while three stent overlap is “the absolute minimum, most of the time—like you—we are much more aggressive.” Greenhalgh further added that this is a “very important matter: the anatomy and the dimensions at the time of deployment are not necessarily the dimensions in the follow-up period, and what fits perfectly in the beginning may not always stay that way.” The use of monitoring for these patients is thus significant to ensure long-term durability. “This is an illustration of how to get the best results, and what the experts are saying”, Greenhalgh concluded.